- Blog
Who do you need to see for Plantar Fasciitis?
Posted on 05-20-2026 in Plantar Fasciitis by Dr. Erik Nilssen
Posted on 05-20-2026 in Plantar Fasciitis by Dr. Erik Nilssen
Plantar fasciitis, which is a condition that leads to moderate to severe pain in the heels of your feet, is often a debilitating ailment. This is one of the more common foot conditions that affects the heels and is caused by inflammation and tension of the plantar fascia tendon.
It is more common in older adults, in people who are obese, and in people who are physically active or have a job requiring a lot of standing or walking. Though it is more common for these individuals, anyone can suffer from it. Here is more information about the diagnosis and who you should see if you think you have this foot condition.
What are the symptoms of plantar fasciitis?
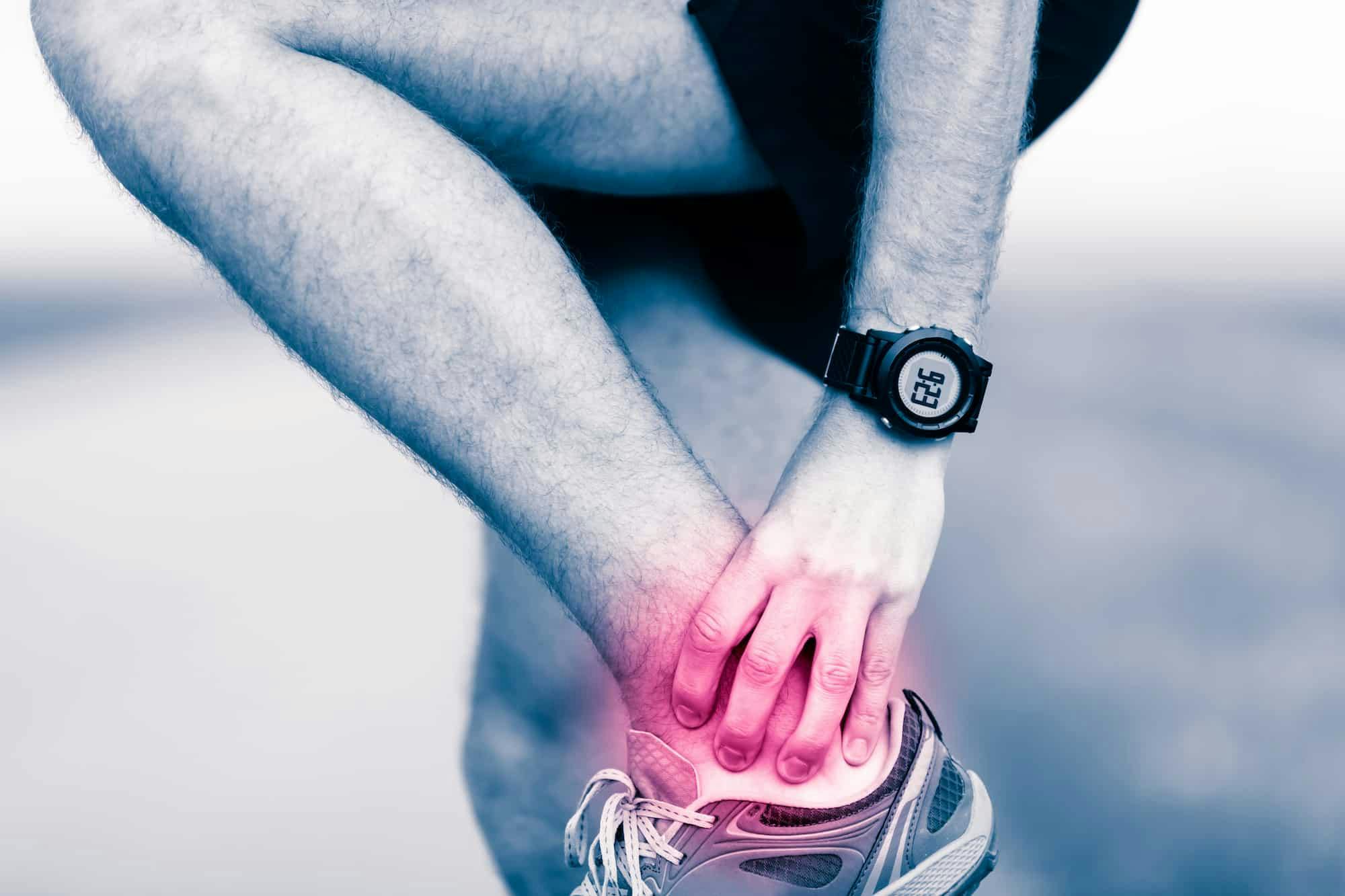
With plantar fasciitis, the most common symptom is pain on the bottom of your foot, usually directly on the heel. It could be a throbbing or stabbing pain when you are standing or walking for a long time or a pins and needles sensation when you have been sitting or lying down and return to a standing position.
Most people who have plantar fasciitis feel moderate to severe pain in the heel while standing, walking, or running, but not during rest. If you also have pain while resting, you might instead have another condition of the foot, such as arthritis. Any time you have pain of the heel and suspect you have plantar fasciitis, though, it’s a good idea to visit your regular doctor first.
How is plantar fasciitis diagnosed?
The first doctor you will see when you think you have plantar fasciitis is your general practitioner. Your doctor will consider the symptoms you're experiencing and will conduct an examination of your foot and heel.
He will look for risk factors of plantar fasciitis, such as having a high arch, having more tenderness near your heel bone, and having worsened pain when flexing the plantar fascia in certain ways.
The next step in diagnosing the condition is to go through a series of x-rays. This allows the doctor to look at the ligaments, tendons, and bones to look for other possible reasons for the pain, such as a fracture, bone spur, or arthritis. You might also be encouraged to get an MRI on the foot and heel.
He will give you a referral to a podiatrist, who is foot specialist, if needed.
What doctor treats plantar fasciitis?
If your general practitioner determines that you have plantar fasciitis, he may advise you to try some at-home-treatments, such as icing, stretching, and taking anti- inflammatory medications at first.
If these at-home methods aren’t helping to relieve your plantar fasciitis pain, your family doctor may refer you to a foot specialist, known as a podiatrist.
This specialist looks at your x-rays or performs them if you haven’t had them yet. He will then give you your treatment options. Most podiatrists begin with non-surgical treatments like stretching exercises, anti-inflammatory pain relievers, massage, and physical therapy. If that isn’t effective, they will recommend custom orthotics to help you find relief, and/or give you night splints.
In the infrequent occasion that at-home treatment methods or therapies provided by your podiatrist don’t help your plantar fasciitis pain, your podiatrist may refer to an orthopedic surgeon to pursue surgical methods as a last resort.

Footwear serves several useful functions, including protecting our feet, cushioning our body weight, providing comfort and, of course, adding a fashionable element to our wardrobe choices. However, selecting the proper footwear can also make a difference in your overall foot health. As you consider those fun new kicks, we encourage you to be mindful of how the right type of shoe can help you avoid injury or further exacerbate existing foot and ankle conditions. Specifically, ill-fitting shoes can be painful and cause issues such as bunions, hammertoes, plantar fasciitis, Lisfranc injuries and more.
May is National Arthritis Awareness Month, and of the more than 100 forms of this painful condition, many can affect the ankle. In fact, almost half of people in their 60s and 70s have arthritis of the foot and/or ankle, but not all of them have symptoms.

North Florida Bone & Joint Specialists continues to embrace the healthcare technology revolution by adding custom, on-site manufacturing of durable medical equipment (DME) from XO Armor Technologies.